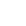NỘI DUNG
Introduction
Buprenorphine is widely prescribed to treat opioid use disorder and has helped millions of people recover from addiction. However, in recent years many patients and dentists have raised concerns about dental damage associated with this medication. Reports of cavities, enamel erosion, and severe oral health problems have sparked an important question: why does buprenorphine cause tooth decay? Understanding the link between this treatment and dental issues is essential for patients who rely on it daily. By exploring the causes, risks, and prevention strategies, patients can continue their treatment safely while protecting their long-term oral health.
What Is Buprenorphine?
Buprenorphine is a prescription medication commonly used to treat opioid use disorder (OUD). It belongs to a class of drugs known as partial opioid agonists, meaning it activates the same receptors in the brain as opioids but produces much weaker effects. This mechanism helps reduce withdrawal symptoms and cravings without creating the intense high associated with drugs like heroin or oxycodone. Because of this unique action, buprenorphine plays a critical role in modern medication-assisted treatment (MAT) programs designed to support long-term recovery from opioid addiction.
Doctors often prescribe buprenorphine as part of a comprehensive treatment plan that includes counseling, behavioral therapy, and medical monitoring. The medication helps stabilize brain chemistry and allows patients to focus on rebuilding their lives while minimizing the risk of relapse. However, like many long-term medications, buprenorphine can have side effects, and one issue that has gained attention in recent years is its potential impact on oral health, including reports of tooth decay and other dental problems.
How Buprenorphine Works in Opioid Treatment
The effectiveness of buprenorphine in treating addiction comes from its ability to partially stimulate opioid receptors in the brain. By doing so, it reduces the severe withdrawal symptoms that occur when someone stops using opioids. At the same time, its ceiling effect limits the level of euphoria it can produce, making it safer and less likely to be abused compared to full opioid agonists.
Many formulations of buprenorphine are designed to dissolve slowly in the mouth, typically under the tongue or inside the cheek. This method, known as sublingual administration, allows the medication to enter the bloodstream efficiently. However, because the tablet or film stays in the mouth for several minutes, it may affect saliva production, oral bacteria, and the overall environment around the teeth—factors that can contribute to dental problems in some patients.
Common Brand Names
Several medications on the market contain buprenorphine, each designed to support recovery from opioid dependence in different ways. Some of the most well-known brands include:
- Suboxone – a combination of buprenorphine and naloxone, widely used in outpatient addiction treatment
- Subutex – contains only buprenorphine and is often prescribed in specific clinical situations
- Zubsolv – a sublingual tablet formulation designed for efficient absorption
- Bunavail – a buccal film that dissolves inside the cheek
- Sublocade – a long-acting injectable form of buprenorphine that provides sustained treatment for a full month
These medications have helped transform the treatment of opioid addiction, giving patients safer and more stable options for recovery. Understanding how buprenorphine works—and how it interacts with the oral environment—is an important first step in recognizing why some patients experience dental complications during treatment.
The FDA Warning About Buprenorphine and Tooth Decay
In recent years, growing reports of dental complications linked to buprenorphine prompted regulatory attention in the United States. Health authorities began noticing a pattern of serious oral health problems among patients using medications that dissolve in the mouth, particularly those prescribed for opioid use disorder treatment. As a result, the U.S. Food and Drug Administration (FDA) issued an official safety communication to inform both patients and healthcare professionals about the potential risks and how to reduce them.
When the FDA Issed the Warning
In January 2022, the FDA released a drug safety communication warning that medications containing buprenorphine and dissolved in the mouth could be associated with serious dental problems. The alert was based on reports submitted through the FDA’s adverse-event monitoring systems and medical literature.
The agency found evidence that sublingual and buccal formulations of buprenorphine—such as tablets placed under the tongue or films inside the cheek—were linked to dental complications. Because of these findings, the FDA required manufacturers to add a new warning about dental risks to prescribing information and patient medication guides for these products.
Despite the warning, the FDA emphasized that buprenorphine remains a critical treatment for opioid addiction and that its benefits still outweigh the potential dental risks when used correctly under medical supervision.
Reported Dental Problems
The safety review identified more than 300 reported cases of dental adverse events associated with buprenorphine medications that dissolve in the mouth, including 131 cases considered serious.
The dental issues reported included:
- Tooth decay and cavities
- Severe enamel erosion
- Oral infections and dental abscesses
- Tooth fractures or fillings falling out
- Partial or complete tooth loss
In some cases, patients required extensive dental procedures such as root canals, crowns, implants, or tooth extractions to treat the damage.
Notably, several reports involved patients who had no previous history of dental disease, suggesting that the medication itself may alter the oral environment in ways that increase the risk of decay.
Because of these findings, healthcare providers are now advised to inform patients about potential dental risks, encourage regular dental visits, and provide guidance on oral hygiene strategies while taking buprenorphine-based medications.
Understanding the FDA warning about buprenorphine and tooth decay helps patients stay informed and take proactive steps to protect their oral health while continuing effective treatment for opioid addiction.
Why Does Buprenorphine Cause Tooth Decay?
Many patients undergoing treatment for opioid use disorder have asked an important question: why does buprenorphine cause tooth decay? While the medication itself is not directly “rotting” teeth, several factors related to how buprenorphine is formulated and used can change the oral environment in ways that increase the risk of cavities and dental damage.
Most forms of buprenorphine—especially those used for addiction treatment—are designed to dissolve slowly in the mouth. During this process, the medication can influence saliva flow, the acidity of the oral environment, and the growth of oral bacteria. Over time, these changes may weaken tooth enamel and allow cavities to develop more easily. Understanding these mechanisms helps explain why some patients experience dental problems during long-term treatment.
Sublingual Medication and Acidic Environment
One of the main reasons behind dental issues is the sublingual administration of buprenorphine. Many medications containing this drug are placed under the tongue or inside the cheek and allowed to dissolve slowly over several minutes.
During this time, the medication remains in direct contact with the teeth and gums. Some formulations may create a slightly acidic environment, which can gradually weaken tooth enamel—the protective outer layer of the teeth. When enamel becomes thinner or damaged, teeth become more vulnerable to cavities, sensitivity, and erosion.
Repeated daily exposure, especially over months or years of treatment, can increase the likelihood of dental deterioration if proper oral care is not maintained.
Reduced Saliva Production (Dry Mouth)
Another important factor is xerostomia, commonly known as dry mouth. Some patients taking buprenorphine report decreased saliva production, which plays a critical role in protecting teeth.
Saliva helps to:
- Neutralize acids in the mouth
- Wash away food particles and bacteria
- Strengthen enamel with natural minerals
When saliva levels drop, the mouth becomes a more favorable environment for cavity-causing bacteria. Without adequate saliva to balance acidity and clean the teeth naturally, tooth decay can develop more easily.
Sugar and Acid in Some Formulations
Certain buprenorphine formulations may contain flavoring agents or ingredients designed to improve taste and absorption. While these components help patients take the medication more comfortably, they can sometimes contribute to an acidic oral environment when the medication dissolves.
Repeated exposure to these substances can gradually weaken dental enamel, particularly when combined with other risk factors such as poor oral hygiene, smoking, or frequent consumption of sugary foods and drinks.
Increased Plaque Bacteria Growth
Changes in the oral environment can also affect the oral microbiome, the community of bacteria naturally present in the mouth. When saliva decreases and acidity increases, plaque bacteria can multiply more easily along the gumline and tooth surfaces.
These bacteria produce acids that slowly break down enamel, leading to cavities and gum irritation. Over time, untreated bacterial activity may cause more serious dental complications, including advanced tooth decay, infections, and gum disease.
See more: Bentonite Clay for Cavities: Natural Tooth Remineralization and Oral Detox
How Common Is Tooth Decay From Buprenorphine?
Dental problems linked to buprenorphine have become an increasing concern in recent years, particularly among patients using medications that dissolve in the mouth. While not everyone who takes buprenorphine-based medications will develop cavities, medical reports and regulatory investigations suggest that the issue is significant enough to require awareness and preventive care. Understanding how frequently these dental problems occur—and who may be most vulnerable—helps patients and healthcare providers take proactive steps to protect oral health during long-term treatment.
Case Reports and FDA Data
Evidence about dental complications related to buprenorphine largely comes from patient reports, clinical observations, and data collected by the U.S. Food and Drug Administration (FDA). In its safety review, the FDA identified more than 300 cases of dental problems associated with buprenorphine medications dissolved in the mouth, including many cases classified as serious.
These reports described a range of oral health issues, such as tooth decay, enamel erosion, infections, and tooth loss. In several instances, patients required extensive dental treatments like root canals, crowns, implants, or tooth extractions to repair the damage. What drew particular attention was that some of the affected patients had no previous history of significant dental disease, suggesting that changes in the oral environment caused by the medication could play an important role.
However, it is important to understand that these numbers represent reported cases, not the total number of people experiencing dental issues. Millions of individuals worldwide use buprenorphine for opioid addiction treatment, and many complete therapy without severe dental complications. This means the overall risk varies depending on individual health factors, oral hygiene habits, and how long the medication is used.
See more: Can Adderall Cause Tooth Decay? Understanding the Connection
Who Is Most at Risk
Although buprenorphine-related tooth decay does not occur in every patient, certain groups appear to have a higher risk of developing dental problems while taking the medication. Several lifestyle and health factors can increase vulnerability to cavities and enamel damage.
People who may face greater risk include those who:
- Already have poor oral hygiene habits
- Experience chronic dry mouth (xerostomia)
- Have a history of dental disease or weak enamel
- Smoke or use tobacco products
- Consume large amounts of sugary or acidic foods and beverages
- Take the medication for long-term treatment
In addition, individuals who rarely visit a dentist or who do not follow preventive oral care practices may not notice early warning signs of dental damage. Over time, untreated plaque buildup and acid exposure can lead to progressive tooth decay and gum disease.
Because of these risk factors, healthcare providers often encourage patients taking buprenorphine to maintain regular dental checkups, practice good oral hygiene, and discuss any changes in oral health with both their doctor and dentist. Early detection and preventive care can significantly reduce the likelihood of severe dental complications while continuing effective addiction treatment.
Symptoms of Buprenorphine-Related Dental Problems
Dental issues associated with buprenorphine treatment may develop gradually, which means many patients do not notice the early signs until the condition has progressed. Because medications containing buprenorphine often dissolve in the mouth, they can alter the oral environment, affecting saliva levels, bacterial growth, and enamel strength. Recognizing the early symptoms of buprenorphine-related dental problems is essential for preventing more serious complications and protecting long-term oral health.
Early Warning Signs
The first symptoms of dental problems linked to buprenorphine use are often subtle and may appear weeks or months after starting treatment. These early indicators usually involve changes in the mouth that signal increased vulnerability to tooth decay and enamel damage.
Common early signs include:
- Tooth sensitivity, especially when consuming hot, cold, or sweet foods
- Persistent dry mouth (xerostomia), which reduces saliva’s protective effects
- Mild gum irritation or inflammation near the gumline
- A chalky or dull appearance of tooth enamel, which may indicate early enamel weakening
- Increased plaque buildup around teeth and gums
At this stage, dental problems are often still reversible or manageable with improved oral hygiene, fluoride treatments, and regular dental checkups. Detecting these symptoms early allows patients to protect their teeth while continuing their buprenorphine therapy safely.
Advanced Dental Damage
If early symptoms are ignored or untreated, the oral changes associated with buprenorphine can lead to more serious dental complications. Over time, reduced saliva and increased bacterial activity can weaken enamel and allow cavities to develop more rapidly.
Advanced signs of dental damage may include:
- Visible cavities or dark spots on teeth
- Noticeable enamel erosion, making teeth appear thinner or worn
- Cracked or chipped teeth due to weakened enamel structure
- Persistent tooth pain or pressure when chewing
- Oral infections or abscesses, which may cause swelling or severe discomfort
In severe cases, patients may require extensive dental treatments such as root canals, crowns, or tooth extractions to repair the damage. These complications highlight the importance of early detection and preventive care for individuals taking buprenorphine-based medications.
Understanding the symptoms of buprenorphine-related dental problems helps patients act quickly when warning signs appear. With proper monitoring, good oral hygiene practices, and regular visits to a dentist, many of these dental issues can be managed effectively without interrupting essential addiction treatment.
See more: Tooth Decay Odor: Why Your Breath Smells “Rotten” & How to Fix It
How to Prevent Tooth Decay While Taking Buprenorphine
Although dental problems have been reported among some patients using buprenorphine, they are often preventable with proper care and awareness. Because many buprenorphine medications dissolve in the mouth, maintaining good oral hygiene and following a few simple precautions can significantly reduce the risk of tooth decay and enamel damage. By adopting preventive habits and working closely with dental professionals, patients can continue benefiting from buprenorphine treatment while protecting their long-term oral health.
Rinse Mouth After Medication
One of the simplest and most effective preventive steps is to rinse the mouth with water after taking buprenorphine. Since many formulations dissolve under the tongue or inside the cheek, residue from the medication can remain in contact with teeth and gums.
Gently rinsing with water helps to:
- Remove remaining medication particles
- Reduce acidity in the oral environment
- Wash away bacteria that contribute to cavity formation
Patients should avoid swallowing the medication prematurely during dissolution, but once it has fully dissolved, rinsing the mouth can help restore a more balanced oral pH and protect tooth enamel.
Wait Before Brushing Teeth
While brushing teeth is essential for preventing cavities, dentists often recommend waiting a short period after the medication has dissolved. Immediately brushing after exposure to an acidic substance can sometimes damage softened enamel.
Instead, patients should:
- Wait about 30 minutes after taking buprenorphine
- Allow saliva to naturally neutralize acids
- Then brush using fluoride toothpaste
This approach helps strengthen enamel while reducing the risk of further irritation to sensitive teeth.
Increase Saliva Production
Saliva plays a crucial role in protecting teeth from decay because it neutralizes acids, removes food debris, and supports the natural remineralization of enamel. However, some individuals taking buprenorphine experience dry mouth (xerostomia).
To help stimulate saliva production, patients can:
- Drink water frequently throughout the day
- Chew sugar-free gum
- Use saliva-stimulating lozenges
- Limit caffeine and alcohol, which may worsen dry mouth
Keeping the mouth well hydrated can greatly reduce the risk of bacterial growth and plaque buildup.
Regular Dental Checkups
Routine visits to a dentist are one of the most important strategies for preventing buprenorphine-related dental problems. Regular dental checkups allow professionals to detect early signs of tooth decay, enamel erosion, or gum inflammation before they become serious.
Dentists may recommend preventive treatments such as:
- Fluoride applications to strengthen enamel
- Dental sealants to protect vulnerable teeth
- Professional cleanings to remove plaque buildup
Patients should inform their dentist that they are taking buprenorphine, as this information helps the dental team tailor preventive care to protect their oral health during treatment.
Use Fluoride Toothpaste
Using fluoride toothpaste daily is a key defense against cavities. Fluoride strengthens tooth enamel and helps repair early stages of mineral loss caused by acid and bacteria.
For best results, patients should:
- Brush twice daily with fluoride toothpaste
- Use a soft-bristled toothbrush to avoid enamel damage
- Consider a fluoride mouth rinse if recommended by a dentist
These simple daily habits can greatly improve resistance to tooth decay and help maintain strong, healthy teeth during long-term buprenorphine therapy.
What Dentists and Doctors Recommend
Healthcare professionals increasingly recognize the importance of protecting oral health in patients receiving buprenorphine treatment for opioid use disorder. While the medication remains a highly effective tool for addiction recovery, dentists and physicians often work together to help patients reduce the risk of tooth decay and other dental complications. By combining medical guidance with preventive dental care, patients can maintain both their recovery progress and their long-term dental health.
Adjusting Medication Forms
In some cases, doctors may consider adjusting the formulation of buprenorphine if a patient experiences significant dental problems. Many dental issues are associated with sublingual or buccal medications that dissolve in the mouth and remain in contact with teeth for several minutes.
When appropriate, healthcare providers may discuss alternatives such as:
- Long-acting injectable buprenorphine, which avoids prolonged contact with teeth
- Different buprenorphine formulations that may dissolve more quickly
- Adjusted dosing strategies that reduce repeated exposure in the mouth
Any medication change must always be carefully supervised by a doctor to ensure that addiction treatment remains effective and stable.
Preventive Dental Treatments
Dentists often recommend additional protective treatments for patients taking buprenorphine-based medications. These preventive measures help strengthen teeth and reduce the risk of enamel erosion and cavities.
Common preventive dental approaches include:
- Professional fluoride treatments to reinforce tooth enamel
- Prescription fluoride toothpaste or mouth rinses
- Dental sealants to protect vulnerable tooth surfaces
- More frequent professional cleanings to remove plaque and bacteria
These treatments can significantly improve resistance to acid damage and support stronger teeth during long-term medication use.
Working With Addiction Specialists
Managing the side effects of buprenorphine therapy often requires collaboration between multiple healthcare providers. Dentists, primary care physicians, and addiction specialists may work together to create a comprehensive plan that protects both recovery and oral health.
This coordinated care can include:
- Monitoring changes in dental health during treatment
- Educating patients about proper oral hygiene practices
- Identifying early signs of tooth decay or gum disease
- Adjusting treatment plans when necessary
By maintaining open communication between medical and dental professionals, patients can receive balanced care that addresses both addiction recovery and long-term dental wellness.
Should You Stop Taking Buprenorphine Because of Tooth Decay?
For many patients, learning about the possible connection between buprenorphine and tooth decay can be concerning. However, health experts strongly emphasize that people should not stop taking buprenorphine without medical supervision. This medication plays a crucial role in treating opioid use disorder, helping reduce cravings, prevent withdrawal symptoms, and significantly lower the risk of relapse or overdose.
Doctors and addiction specialists widely agree that the benefits of buprenorphine treatment often outweigh the potential risks to oral health. For individuals recovering from opioid addiction, stopping medication suddenly can lead to serious consequences, including withdrawal symptoms and a higher chance of returning to opioid use. Because of these risks, treatment decisions should always be made in consultation with a qualified healthcare provider.
Instead of discontinuing the medication, many experts recommend focusing on preventive dental care and early management of oral health problems. Dentists and doctors can work together to monitor symptoms of dental damage, recommend protective strategies, and adjust treatment when necessary. Simple habits—such as maintaining good oral hygiene, rinsing the mouth after medication, and attending regular dental checkups—can greatly reduce the risk of cavities.
In some cases, healthcare providers may also discuss alternative treatment options, such as different buprenorphine formulations or long-acting injectable medications that do not dissolve in the mouth. These options can help minimize prolonged contact between the medication and the teeth while still supporting effective addiction recovery.
Ultimately, the safest approach is to treat oral health issues while continuing medically supervised buprenorphine therapy. With proper guidance from doctors and dentists, most patients can protect their teeth and maintain the stability that this life-saving medication provides during recovery.
The Future of Safer Addiction Medications
As awareness grows about the link between buprenorphine treatment and certain dental health concerns, researchers and pharmaceutical companies are actively working to improve the safety and convenience of medications used for opioid use disorder. The goal is not only to maintain the life-saving benefits of addiction therapy but also to reduce potential side effects that may affect oral health and overall well-being.
One promising development is the expansion of long-acting buprenorphine formulations. Medications such as monthly injectable treatments deliver a controlled dose of buprenorphine directly into the bloodstream without dissolving in the mouth. Because these formulations bypass the sublingual route, they eliminate prolonged contact between the medication and the teeth, which may reduce the risk of tooth decay and enamel erosion associated with oral tablets or films.
Researchers are also exploring improved medication delivery systems that minimize exposure of the teeth to active compounds while maintaining effective absorption. Advances in pharmaceutical technology may lead to new formulations of addiction medications that dissolve more quickly, maintain a neutral oral pH, or include protective ingredients designed to support oral health.
Another important focus for the future is patient education and preventive care. Healthcare systems are increasingly encouraging collaboration between addiction specialists, dentists, and primary care providers. This integrated approach helps patients receive guidance on oral hygiene practices, regular dental monitoring, and strategies to prevent medication-related dental complications.
In addition, ongoing research into next-generation treatments for opioid addiction may expand therapeutic options beyond current medications. Scientists continue to study new compounds, alternative delivery methods, and personalized treatment approaches that improve both treatment effectiveness and patient safety.
While buprenorphine remains one of the most effective tools for managing opioid dependence, the future of addiction medicine is moving toward treatments that balance recovery support, patient comfort, and long-term health protection. As these innovations continue to develop, patients can expect safer and more refined therapies that support recovery while minimizing potential side effects.
Conclusion
Understanding why does buprenorphine cause tooth decay helps patients take proactive steps to protect their oral health while continuing essential treatment for opioid use disorder. Although medications like buprenorphine can affect the oral environment—through dry mouth, prolonged contact with teeth, and bacterial growth—the risk of dental problems can often be reduced with proper oral hygiene, regular dental checkups, and simple preventive habits. Most importantly, patients should never stop treatment without medical advice. With the right care and guidance from healthcare professionals, it is possible to manage dental risks while safely benefiting from buprenorphine therapy during recovery.